
Holland Bloorview’s psychopharmacology clinic delivers individualized treatment to families that need it most
Only one of few in Ontario, Holland Bloorview’s psychopharmacology clinic serves children and youth with complex medical, mental health and developmental differences who require medication management as part of their overall treatment plan. As the complexity of clients’ needs continue to increase – an evolving challenge observed across the health-care system – the clinic has adapted its care model over the years by expanding its supports for families through its interprofessional team and holistic approach to treatment.
Consisting of specialized physicians, a nurse practitioner (NP), registered nurses (RN), behaviour analysts, behaviour technician and pharmacists, the clinic is best positioned to provide a tailored and responsive approach to treatment for families with urgent needs. Interfering behaviours such as aggression and anxiety, paired with food insecurity and critical respite needs are becoming increasingly common challenges faced by clients and their families.

“If not us, then who?” says Josh Scroggy, clinical operations manager, autism services and psychopharmacology. “The reality is that the health-care system has become a reactive system. In the absence of proactive clinics to address the evolving complexity of children’s needs, families experience escalating urgency as they wait for care. Through this clinic, we’re making it our focus to see kids who may have no other place to go.”
For the past two years, the psychopharmacology clinic received an average of 100 referrals (including from the hospital’s Extensive Needs Service) – this year it received approximately 138 and saw about 90 new clients. To help reduce a waitlist of clients across Ontario, innovative approaches such as NP-led care and its embedded transition clinic are focused on improving access without compromising individual treatment.
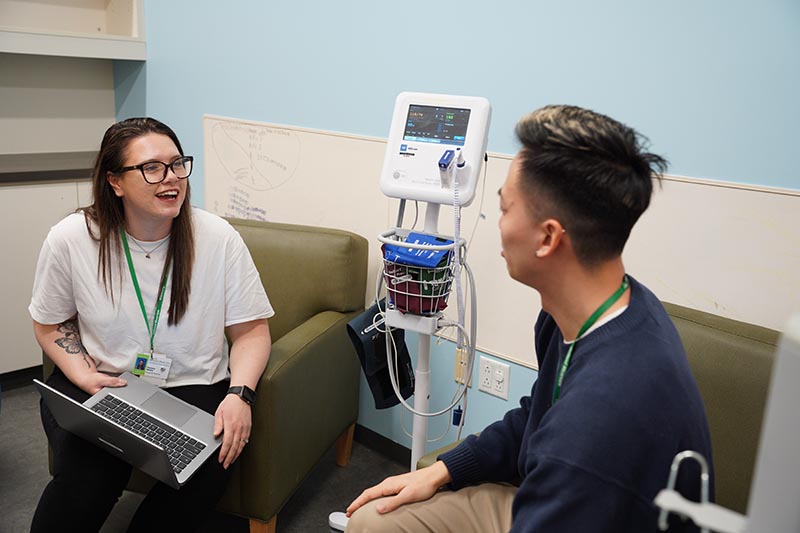
NP-led approach leads to enhanced outcomes
Embedded in the psychopharmacology clinic is its NP-led clinic. As the Most Responsible Provider (MRP), the NP collaborates with an interprofessional team to assess, diagnose and treat clients, enabling all providers to work to their full scope allowing for comprehensive holistic care. Bridget Doan, pediatric nurse practitioner, psychotherapist in the psychopharmacology clinic shares: “One of the most striking things about the families we work with is their love for their children and their willingness to think outside the box and try creative approaches to care – both medication- and therapy-wise. They are truly the experts on their children.”
Countless families have gratefully expressed the impact that an NP at this clinic had on them. One family shares: “When my son was barreling into crisis, a nurse practitioner was the one who changed everything. She had the wisdom to understand what our family needed, the skill and knowledge to provide that support and the compassion and determination to make sure that anything she couldn’t do herself got done by someone who could.”
Doan reflects: “There is nothing more rewarding than when the right combination of medication and therapeutic intervention comes together to change someone’s life. To see a client in follow up a few months later reaching their goals, such as feeling confident in their schoolwork, making friends, or gaining new communication skills – it stays with you.”
Transitioning children back into their communities safely
The safe discharge of a client back into their community is paramount, especially when life-changing medication is involved. The transition clinic is another innovative care path embedded into the psychopharmacology clinic – anchored by a strong client and family-centered approach.
“Our RNs go above and beyond the work,” says Scroggy. “While we’re not an acute care service, they answer pressing calls with compassion and expertise. They build the trust of the families we see.”
From a safety perspective, the clinic’s team of experts have built in processes that see minimal Code White calls, which are used to support rare situations involving escalated behaviour. “We know our kids. No family comes onsite without the team understanding who needs to be present, what activities they enjoy and what may cause them stress,” says Doan.
She also makes note of medication safety, expressing that visits include a review of all medication – what is taken, how it’s taken, the benefits, the side effects and if it’s stored safely at home. “We encourage our clients and families to learn the names of their medications and the reasons why they take them.”

The hospital has the expertise, the people and the power to transform disability care, everywhere. By combining innovation with compassionate, family-centred care, the psychopharmacology clinic continues to reshape and evolve what responsive care can look like, while ensuring children with complex needs – and their families – are seen, supported and empowered.
“Our model of care puts safety, dignity and families first – long after a clinic visit ends,” says Scroggy.
By Ashley Cruz
Photos by Will Lam